Living with heart disease brings challenges that are hard to fully appreciate until you’ve experienced them firsthand. In this post, I’m sharing my personal journey with AV block, amiodarone, and ultimately receiving a leadless pacemaker — in the hope that it might help someone else navigating a similar path. Please note that I do not have a medical background.
Atrioventricular Block
I was recently admitted to A&E after a faint and subsequently diagnosed with atrioventricular block. AV block refers to a condition where there is a delay or interruption in the transmission of electrical signals from the upper chambers (atria) to the lower chambers (ventricles) of the heart. This can result in a slower heart rate or even a complete block of electrical impulses, which can be dangerous and lead to symptoms such as dizziness, fainting, or heart failure. AV block and tachycardia are not directly related, and their treatments can be different depending on the underlying cause. I already had an ICD implanted in April 2020 after a suspected cardiac arrest caused by ventrical tachycardia (ventricular tachycardia is a fast heart rate that originates in the ventricles of the heart), whilst out riding my bike The unexpected diagnosis – ARVC and this was extracted and replaced by an S-ICD in February 2023 Living with ICD complications.
Amioderone
In late November 2022, I was prescribed amiodarone to treat my irregular heart rhythm, specifically to reduce my ectopic burden of PVCs (premature ventricular contractions) in preperation for my S-ICD installation in February 2023. My PVCs are estimated to make up more than 30% of my heartbeats, meaning that over 3 in every 10 beats are ectopic. However, it’s important to note that in some cases, amiodarone can actually cause or worsen a condition called atrioventricular block. This occurs because the medication affects the heart’s conduction system, which can cause delays or interruptions in the transmission of electrical signals, leading to AV block becoming more prominent or apparent.
Its potency stems from its ability to block multiple types of ion channels in the heart, which helps to stabilize the heart’s electrical activity and prevent abnormal rhythms. Additionally, amiodarone has a long half-life, meaning that it remains in the body for an extended period of time, allowing for sustained therapeutic effects. However, it can also result in significant side effects. The potency of amiodarone requires close monitoring by a doctor to ensure that the medication is effective while minimizing the risk of side effects.
The half-life of amiodarone can range from 20 to 100 days, depending on various factors such as age, gender, and overall health. This means that it can take several weeks or even months for the body to eliminate half of the dose of amiodarone taken.
Side Effects of Amiodarone
Some of the side effects included but are not limited to:
| Low Risk | Medium Risk | High Risk |
|---|---|---|
| Blurred vision | Hypotension | Abnormal hepatic function tests |
| Corneal deposits | Nausea | Bradycardia |
| Dermatological reaction | Constipation | Heart block |
| Gastrointestinal signs and symptoms | Cough | Involuntary body movements |
| Photophobia | Dizziness | Neurotoxicity |
| Phototoxicity | Dyspnea | Paresthesia |
| Skin photosensitivity | Fatigue | Solar dermatitis |
| Visual halos around lights | Abnormal gait | Tremor |
| Xerophthalmia | Asthenia | Visual disturbance |
| Malaise | Blue-gray skin pigmentation | |
| Persistent ventricular tachycardia | Hypersensitivity pneumonitis | |
| Pneumonitis | Interstitial pneumonitis | |
| Pulmonary toxicity | ||
| Pulmonary alveolitis |
Leadless Pacemaker
A leadless pacemaker is a small device that is used to regulate the heartbeat. It is about the size of a large vitamin capsule, with a weight of only 2 grams.

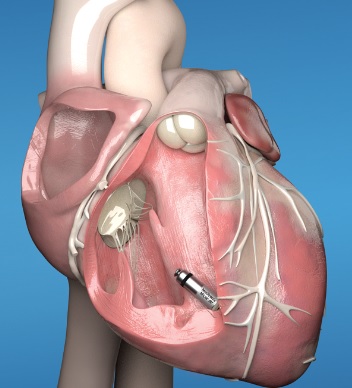
This pacemaker is designed to be placed inside the heart, so there are no wires that need to be threaded through the veins like traditional pacemakers and that of the ICD that caused my SVC obstruction (Living with ICD complications) as a result of lead installation. Instead this pacemaker is inserted into the heart via a small incision in the upper leg and guided into place through the femoral vein. Once in place, the pacemaker uses electrical impulses to regulate the heartbeat, just like a traditional pacemaker. The pacemaker can last for up to 14 years, and can be monitored remotely by healthcare professionals to ensure that it is working properly, albeit this consumes the battery faster.
Pacemaker Settings and AV Synchrony
When a pacemaker is installed, the settings can be adjusted to meet the specific needs of the patient. One common setting is the minimum ventricular rate, which determines the lowest rate at which the pacemaker will stimulate the heart to beat. In my case, the pacemaker is set to maintain a minimum ventricular rate of 40 beats per minute.
Another important setting in pacemakers is called AV synchrony, which will address the AV block symptoms I have experienced. AV synchrony ensures that the atria (the top chambers of the heart) and ventricles (the bottom chambers of the heart) work together properly. Specifically, it ensures that the ventricles contract after the atria have finished contracting, which helps to optimize the blood flow through the heart.
Advanced Pacemaker Features
In addition to these basic functions, modern pacemakers have a variety of advanced features. For example, they can automatically adjust the pacing rate based on the patient’s activity level or other physiological signals. In trial at the moment is a pacemaker that can communicate with other implanted devices, such as defibrillators (S-ICD), to coordinate their actions and optimize the patient’s heart function. If you want to learn about this new modular technology and see how the device is implanted, take a look here Boston Scientific Emblem Modular S-ICD / Leadless Pacemaker.